Trichotillomania: Understanding the Disorder, Its Causes, Severity Levels, and Treatment Options
Trichotillomania is a psychological disorder characterized by recurrent, irresistible urges to pull out one’s own hair, commonly affecting the scalp, eyebrows, eyelashes, or other body areas. Although often misunderstood or minimized, this condition can deeply affect emotional well-being, self-esteem, interpersonal relationships, and overall quality of life.
Classified within the group of Obsessive-Compulsive and Related Disorders, trichotillomania is not simply a “bad habit” or lack of self-control. Rather, it is a complex mental health condition that involves difficulties in impulse regulation, emotional processing, and behavioral control. Understanding its nature is essential for reducing stigma and promoting effective treatment.
This article offers a comprehensive, evidence-based overview of trichotillomania, including diagnostic criteria, severity levels, causes and risk factors, treatment approaches, and a lifespan perspective, while emphasizing hope, recovery, and personal strengths.
Historical Context and Terminology
Historically, trichotillomania was poorly understood and often dismissed as a nervous habit or a sign of weak willpower. The term itself was introduced in the late 19th century, but only in recent decades has the disorder been properly recognized within psychiatric classification systems.
With the publication of the DSM-5, trichotillomania gained clearer diagnostic criteria and was formally placed among obsessive-compulsive and related disorders, reinforcing its neurobehavioral and psychological foundations. This shift has helped validate patient experiences and guide more effective, compassionate interventions.
What Is Trichotillomania?
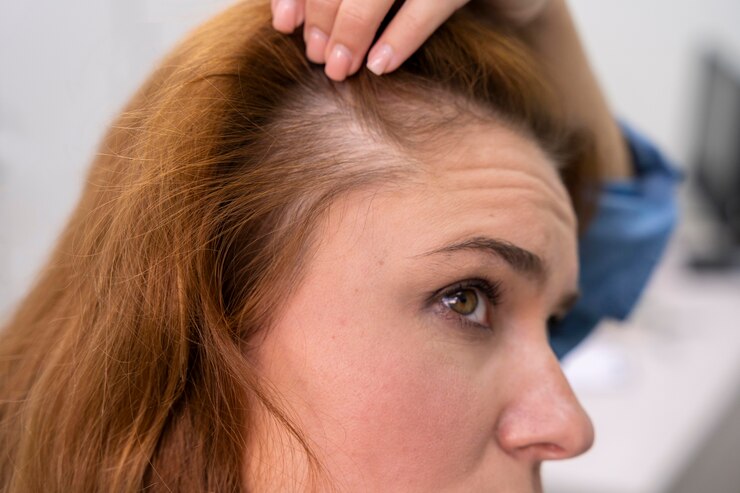
Trichotillomania involves repetitive hair-pulling behaviors that result in noticeable hair loss and significant distress or impairment. Individuals may pull hair consciously, in response to emotional tension, or automatically, often during periods of distraction, boredom, or stress.
Although the behavior may temporarily reduce internal tension or provide a sense of relief, it is usually followed by shame, frustration, or guilt. Over time, this cycle reinforces the behavior, making it increasingly difficult to stop without professional support.
DSM-5 Diagnostic Criteria Explained
According to the DSM-5, trichotillomania is diagnosed when an individual presents recurrent pulling out of one’s hair resulting in hair loss, repeated attempts to decrease or stop the behavior, and clinically significant distress or impairment in social, occupational, or other important areas of functioning.
The symptoms cannot be attributed to another medical condition, such as a dermatological disorder, nor better explained by another mental disorder. Importantly, diagnosis requires careful clinical evaluation to differentiate trichotillomania from conditions involving hair loss without compulsive behavior.
Severity Levels of Trichotillomania
The severity of trichotillomania varies widely and is best understood on a continuum rather than as a single presentation.
In mild cases, hair pulling occurs infrequently, causes minimal visible hair loss, and has limited impact on daily functioning. Individuals may still feel distress but retain a relatively high level of control.
Moderate cases involve more frequent urges, noticeable hair loss, and increased emotional distress. Individuals may begin avoiding social situations or using strategies to conceal hair loss.
Severe trichotillomania is marked by persistent, uncontrollable pulling, significant alopecia, and substantial impairment in social, academic, or occupational functioning. Emotional suffering, shame, and avoidance behaviors become more pronounced.
In profound cases, the disorder dominates daily life, severely affecting self-image, mental health, and quality of life, often co-occurring with depression, anxiety, or other obsessive-compulsive symptoms.
Core Characteristics and Behavioral Patterns
Individuals with trichotillomania often experience a rising sense of tension, anxiety, or discomfort before pulling hair, followed by relief, gratification, or calm afterward. Over time, this relief reinforces the behavior, creating a compulsive loop.
Some individuals engage in focused pulling, fully aware of the act, while others experience automatic pulling with little conscious awareness. Both patterns can coexist and vary depending on emotional states and environmental contexts.
Causes and Risk Factors
The etiology of trichotillomania is multifactorial and involves a complex interaction of biological, psychological, and environmental influences.
Genetic vulnerability plays a role, as individuals with a family history of obsessive-compulsive disorders, anxiety, or impulse-control disorders show increased risk. Neurobiological factors, including differences in brain circuits related to habit formation and emotional regulation, have also been identified.
Psychological factors such as anxiety, emotional dysregulation, perfectionism, trauma, and chronic stress significantly contribute to the development and maintenance of the disorder. Many individuals report hair pulling as a coping mechanism for overwhelming emotions.
Environmental and developmental factors, including early life stress, family dynamics, and learned coping behaviors, further shape symptom expression.
Emotional and Psychosocial Impact
Beyond physical hair loss, trichotillomania profoundly affects emotional health. Many individuals struggle with low self-esteem, body image dissatisfaction, shame, and fear of judgment. Social withdrawal is common, particularly when visible hair loss leads to embarrassment or avoidance of intimacy.
These emotional consequences often reinforce the disorder, highlighting the importance of addressing both behavior and underlying emotional needs in treatment.
Evidence-Based Interventions
Effective treatment for trichotillomania relies on evidence-based, individualized approaches that address behavioral, emotional, and cognitive components.
Cognitive-behavioral therapy, particularly Habit Reversal Training (HRT), is considered the gold standard. This approach helps individuals identify triggers, increase awareness of pulling behaviors, and develop alternative responses to urges.
Acceptance and Commitment Therapy (ACT) and emotion regulation strategies further support long-term change by reducing avoidance and increasing psychological flexibility.
Role of Medication
Although no medication is universally effective, certain pharmacological options may be helpful for some individuals, particularly when trichotillomania co-occurs with anxiety or depression. Selective serotonin reuptake inhibitors and other agents may be considered as part of a comprehensive treatment plan under psychiatric supervision.
Family and Social Support
Support from family members and close relationships plays a crucial role in recovery. Psychoeducation helps loved ones understand the disorder, reduce judgment, and create a supportive environment that encourages treatment adherence and emotional safety.
Trichotillomania Across the Lifespan
In childhood, hair pulling may initially appear as a self-soothing behavior, often emerging during periods of stress or transition. Early intervention can prevent symptom escalation.
During adolescence, increased self-awareness and social pressures may intensify distress and concealment behaviors. In adulthood, responsibilities and chronic stress can maintain symptoms, while untreated cases may persist for years.
In later life, trichotillomania may fluctuate with life changes, health challenges, or emotional stressors, reinforcing the need for ongoing coping strategies and support.
Prognosis and Recovery
Although trichotillomania can be chronic, many individuals experience significant improvement with appropriate treatment. Recovery does not necessarily mean the complete absence of urges, but rather the ability to manage them effectively without significant distress or impairment.
Final Considerations
Trichotillomania is a legitimate and treatable mental health condition. With proper diagnosis, evidence-based intervention, and compassionate support, individuals can regain control, rebuild self-confidence, and improve their quality of life.
If you or someone you know is struggling with hair-pulling behaviors, seeking professional help is a powerful and courageous step. Recovery is possible, and a life guided by self-compassion, resilience, and well-being is within reach.
Read Also
For further information and reliable guidance, consider exploring resources from the American Psychiatric Association, the CDC, the National Institute of Mental Health, The TLC Foundation for Body-Focused Repetitive Behaviors, and peer-reviewed clinical literature on obsessive-compulsive and related disorders.

